Get Healthy!
Staying informed is also a great way to stay healthy. Keep up-to-date with all the latest health news here.
17 Mar
Early Exposure to “Forever Chemicals” May Affect Teen Bone Health
A new study suggests exposure to PFAS “forever chemicals” early in life may affect bone development during adolescence, with stronger effects seen in girls.
16 Mar
Loneliness in Perimenopause Linked to Changes in Brain Health
A new study shows loneliness and social isolation together may sharply increase the risk of memory and thinking problems during perimenopause.
13 Mar
Ultra-Processed Foods May Be Bad for Your Bones, Study Finds
Eating too many ultra-processed foods lowers bone mineral density and raises the risk of hip fracture, researchers warn.
Norovirus Sickens Close to 200 People on Caribbean Cruise
A Caribbean vacation took an unpleasant turn for dozens of cruise passengers after a stomach virus spread across their ship.
Nearly 200 people aboard a Princess cruise vessel became sick with norovirus during a recent trip, according to the U.S. Centers for Disease Control and Prevention (CDC).
The agency said 193 people fell ill dur...
- HealthDay Staff HealthDay Reporter
- |
- March 17, 2026
- |
- Full Page
Federal Judge Pauses Kennedy’s Changes to Childhood Vaccine Schedule
A federal judge has stopped a major effort to change the nation’s childhood vaccine schedule.
The ruling, issued Monday in Massachusetts, blocks U.S. Health Secretary Robert F. Kennedy Jr.’s plan to revise vaccine recommendations for children.
The decision stems from a lawsuit brought by several medical groups again...
- HealthDay Staff HealthDay Reporter
- |
- March 17, 2026
- |
- Full Page
Listening to Music for 24 Minutes May Ease Anxiety, Study Finds
A short music session may help ease anxiety and researchers say there’s a "sweet spot" for how long to listen.
A clinical trial found that listening to specially designed music for 24 minutes can significantly reduce anxiety symptoms. The music was paired with auditory beat stimulation (ABS), a type of sound pattern meant to influenc...
- HealthDay Staff HealthDay Reporter
- |
- March 17, 2026
- |
- Full Page
Cream Cheese Recall Upgraded Over Listeria Risk, FDA Says
Health officials are warning consumers about a cream cheese recall that has been raised to the most critical level due to possible bacterial contamination.
The U.S. Food and Drug Administration (FDA) said certain cream cheese products made by Made Fresh Salads Inc. may contain Listeria monocytogenes, a bacteria that can cause seve...
- HealthDay Staff HealthDay Reporter
- |
- March 17, 2026
- |
- Full Page
New Moms Need Weeks Of Monitoring To Catch Post-Pregnancy Complications, Study Argues
New mothers need to be monitored weeks after delivery for pregnancy complications, a new study suggests.
About 40% of pregnancy complications would have been missed had doctors not kept tabs on new moms for six weeks following delivery, researchers reported March 16 in the Canadian Medical Association Journal.
Typically, hea...
- Dennis Thompson HealthDay Reporter
- |
- March 17, 2026
- |
- Full Page
VR Effective In Educating Patients About Upcoming Procedures
Imagine a doctor offering you a virtual reality headset to help explain an upcoming procedure.
It turns out such an explanation might go farther to easing your worries than the usual handout leaflet, researchers reported Friday at a meeting in London of the European Association of Urology (EAU).
Patients said they felt less anxious a...
- Dennis Thompson HealthDay Reporter
- |
- March 17, 2026
- |
- Full Page
Prebiotic Eases Arthritis Pain, Trial Finds
Making your gut happy might help angry arthritis-affected joints, a new study says.
A prebiotic fiber supplement helped ease pain in people with knee arthritis, researchers recently reported in the journal Nutrients.
The results suggest that improving gut health could be a new way to treat arthritis, researchers said.
...
- Dennis Thompson HealthDay Reporter
- |
- March 17, 2026
- |
- Full Page
Drug Protects Against Chemo-Caused Bleeding, Trial Shows
An already approved drug can help protect cancer patients against excessive bleeding caused by chemotherapy, a new study says.
Chemotherapy-induced thrombocytopenia occurs when chemo destroys platelet-producing bone marrow cells, increasing a person’s risk of dangerous bleeding.
But the injectable drug romiplostim (Nplate) can ...
- Dennis Thompson HealthDay Reporter
- |
- March 17, 2026
- |
- Full Page
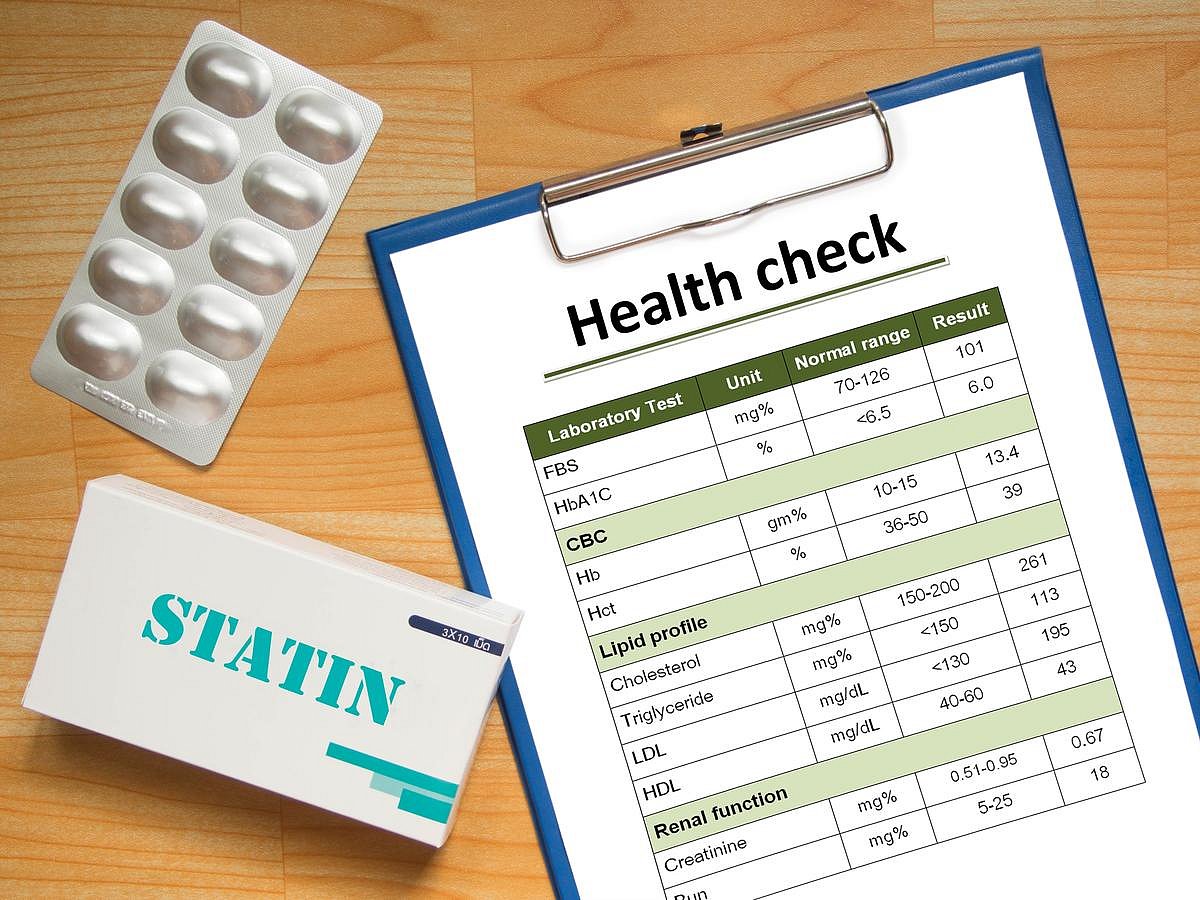
Cholesterol Needs Lifelong Management, New Heart Guidelines Say
Heart experts are calling for a full-court press against cholesterol, including lifelong screening and treatment, a set of new guidelines says.
Blood testing for cholesterol should start in childhood, and take place at least every five years to track each person’s heart health risk, the American College of Cardiology and the American...
- Dennis Thompson HealthDay Reporter
- |
- March 17, 2026
- |
- Full Page
Insurance Red Tape Delays Crucial Heart Failure Drug Prescriptions, Study Finds
Insurance requirements could keep people from getting life-saving heart medications in a timely fashion, a new study says.
Prescriptions for heart failure medications take two to six times longer to fill if insurance companies require prior authorization — a process that requires doctors to obtain insurers’ approval before a tr...
- Dennis Thompson HealthDay Reporter
- |
- March 17, 2026
- |
- Full Page
Officials Examine Deaths After Plasma Donations in Winnipeg
Canadian health officials are investigating the deaths of two people who donated plasma at private clinics in Winnipeg, Manitoba.
The deaths happened about three months apart, one in October 2025 and the other in January 2026, according to Health Canada, the federal agency that regulates plasma donation clinics.
One of the donors who...
- HealthDay Staff HealthDay Reporter
- |
- March 16, 2026
- |
- Full Page
New Flu Strain Weakened This Year’s Vaccine Protection, CDC Says
Flu activity in the United States is finally slowing down, but health experts say this year’s flu vaccine didn't offer as much protection as officials hoped.
New data from the U.S. Centers for Disease Control and Prevention (CDC) shows that the vaccine was only about 25% to 30% effective in preventing illness serious enough to send a...
- HealthDay Staff HealthDay Reporter
- |
- March 16, 2026
- |
- Full Page
New EPA Rule Could Loosen Limits on Medical Device Sterilization Gas Emissions
The U.S. Environmental Protection Agency (EPA) is proposing to loosen limits on emissions of ethylene oxide, a gas used to sterilize many medical devices that is also linked to cancer.
The proposal, announced Friday, would ease pollution rules for about 90 commercial sterilization facilities nationwide.
Ethylene oxide plays an import...
- HealthDay Staff HealthDay Reporter
- |
- March 16, 2026
- |
- Full Page
Food Stamp Users Fight Restrictions on Soda and Sweets
Five people who qualify for food stamps are suing the U.S. Department of Agriculture (USDA) because new rules stop them from using their benefits to buy sugary drinks and candy.
The lawsuit, filed Wednesday in federal court in Washington, D.C., argues the limits are illegal and make it harder for families to manage their food and health ne...
- HealthDay Staff HealthDay Reporter
- |
- March 16, 2026
- |
- Full Page
Loneliness, Social Isolation Impact Brain Health Among Women Entering Menopause
Loneliness can impact a woman’s brain health as she begins menopause, a new study says.
Loneliness and social isolation are both linked to the cognitive decline a woman feels as she begins to transition into menopause, researchers recently reported in the journal Menopause.
Further, women experiencing both loneliness a...
- Dennis Thompson HealthDay Reporter
- |
- March 16, 2026
- |
- Full Page
Poor Hearing Makes It Harder For Blind Folks To Navigate
Poor hearing can dramatically impact a blind person’s ability to navigate and move around in their daily life, a new study says.
People who’ve gone blind can still use hearing to help them avoid obstacles and reach destinations.
But blind people who also have experienced hearing loss have more difficulty perceiving and lo...
- Dennis Thompson HealthDay Reporter
- |
- March 16, 2026
- |
- Full Page
Other People's Opinions Can Shape How You Feel About Pain, Mental Challenges
You’re waiting for a vaccination. The person ahead of you stumbles out, groaning about how painful the shot was.
Could hearing that make your own injection hurt worse?
Yes, a new study says.
What others say about an experience – be it a vaccination, or a job interview, or a college course – can shape how it ac...
- Dennis Thompson HealthDay Reporter
- |
- March 16, 2026
- |
- Full Page
Exercise Promotes Release Of Brain-Boosting Protein, Study Shows
It’s long been known that exercise improves a person’s brain health – and researchers now think they better understand at least one of the factors at play.
Just one 15-minute session of aerobic exercise floods the brain with brain-derived neurotrophic factor (BDNF), a protein known to support the health of new and existin...
- Dennis Thompson HealthDay Reporter
- |
- March 16, 2026
- |
- Full Page
One-Third Of U.S. Parents Worried Their Young Driver Could Cause A Car Crash
Many U.S. parents are worried that their teen or young adult is going to cause a wreck through their unsafe driving, a new survey says.
About 1 in 3 parents worry that their young driver could cause a motor vehicle accident, according to the University of Michigan Health C.S. Mott Children’s Hospital National Poll on Children’s...
- Dennis Thompson HealthDay Reporter
- |
- March 16, 2026
- |
- Full Page
Medical Debt Forces Many to Skip Essential Health Care
People who’ve racked up medical debt are more likely to skip health care that could prevent future illnesses, a new study reports.
Folks weighed down by hospital and doctor bills are much more likely to delay medical, dental and mental health care, researchers reported in the Journal of General Internal Medicine.
&ldqu...
- Dennis Thompson HealthDay Reporter
- |
- March 16, 2026
- |
- Full Page