Get Healthy!
Staying informed is also a great way to stay healthy. Keep up-to-date with all the latest health news here.
05 Jun
How Brain Surgery Helped an Illinois Mom Grow Her Family
When medication stopped working and a brain tumor stood in the way of another pregnancy, one Illinois mom faced a life-changing decision.
04 Jun
Nearly 1 in 5 Young People Turn to AI Chatbots for Mental Health Advice
A new study finds that 19.2% of adolescents use AI chatbots when feeling sad, nervous, or stressed, and most do not tell their parents they are seeking mental health advice from AI.
03 Jun
Just 90 Minutes of Strength Training a Week Linked to Longer Life
A study of more than 147,000 adults found that about 90–119 minutes of strength training per week was linked to a lower risk of death from all causes, from heart disease and brain diseases.
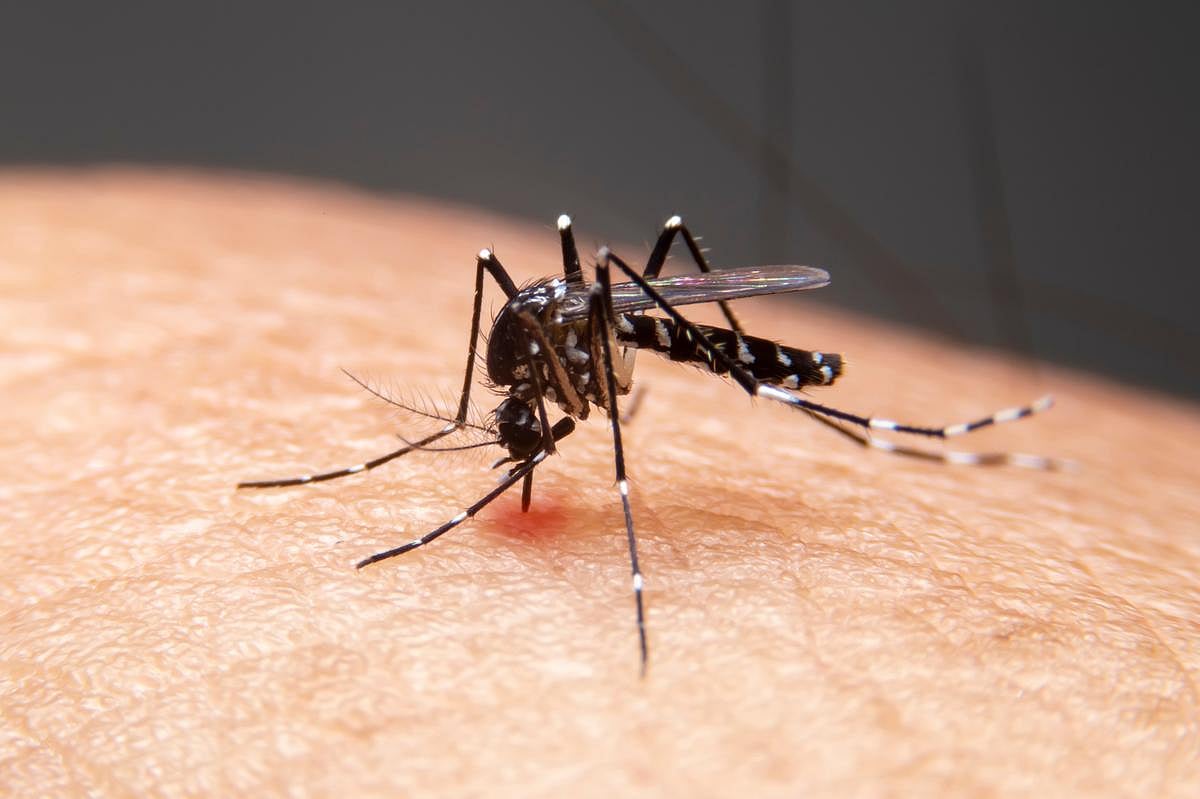
Dengue Is No Longer Just A Travel Risk — What Google’s Mosquito Plan Could Mean For Your Summer
This is not science fiction or some perverse prank.
A Silicon Valley tech giant is seeking federal approval to release up to 64 million sterilized male mosquitoes in California and Florida over the next two years.
The aim?
To drive down the population of Aedes aegypti mosquitoes, which transmit infectious d...
- Andria Park Huynh HealthDay Reporter
- |
- June 5, 2026
- |
- Full Page
Brain Surgery For Pituitary Tumor Helps Illinois Mom Have Second Baby
A suburban Chicago woman who feared she might never have another child is now celebrating a growing family after brain surgery at Northwestern Medicine.
After the birth of her first daughter in 2022, Lisa Fasone began experiencing postpartum hormonal issues.
"My menstrual cycle never came back. After I had my baby and I was done nurs...
- HealthDay Staff HealthDay Reporter
- |
- June 5, 2026
- |
- Full Page
Spinal Cord Stimulation May Restore Arm Strength After Stroke
Electrical stimulation of the spinal cord might improve arm function among people who’ve suffered a stroke, pilot clinical trial results say.
Seven stroke survivors with profound muscle weakness had an average 32% increase in their arm strength after receiving spinal cord stimulation (SCS), researchers reported June 4 in the journal ...
- Dennis Thompson HealthDay Reporter
- |
- June 5, 2026
- |
- Full Page
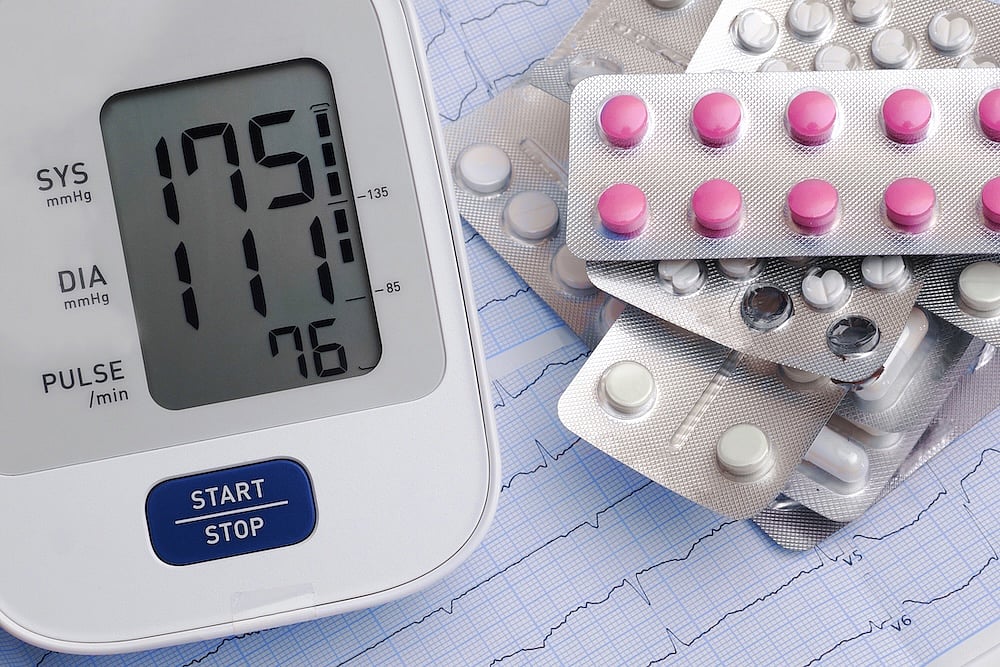
Popular Blood Pressure Meds Linked To Kidney Damage Risk In Type 2 Diabetes
A common class of blood pressure medications might contribute to kidney damage among people with type 2 diabetes, a new study says.
Dihydropyridine calcium-channel blockers (DCCBs) work by relaxing blood vessels, and are frequently used as second-line therapies in people with diabetic kidney disease (DKD), researchers said.
But patie...
- Dennis Thompson HealthDay Reporter
- |
- June 5, 2026
- |
- Full Page
Too Much Sitting In Pregnancy Doubles Risk Of Complications
In the old days, expecting mothers were encouraged to take it easy as much as possible.
But that advice had it completely backward, a new study says.
There are higher odds of pregnancy complications for women who spend more time sitting, compared to those who include even light activity in their daily routine, researchers reported re...
- Dennis Thompson HealthDay Reporter
- |
- June 5, 2026
- |
- Full Page
Two-Pill Combo Offers Hospital-Free Leukemia Treatment Option For Older Adults With AML
An already available two-pill combo treats leukemia just as well as IV drugs, which should make cancer treatment easier on older adults, a new clinical trial has concluded.
The combo – decitabine-cedazuridine and venetoclax – showed strong response rates and survival outcomes among older adults with acute myeloid leukemia (AML)...
- Dennis Thompson HealthDay Reporter
- |
- June 5, 2026
- |
- Full Page
Poll Finds Broad Support For Stricter Regulations On Ultra-Processed Foods
Top food researchers have teamed up on a special issue of the American Journal of Public Health to push policymakers for stricter action on ultra-processed foods (UPFs).
In a press call ahead of the issue's release, food politics scholar Marion Nestle underscored its "Do policy!" message accompanied by new polling showing "broad c...
- Andria Park Huynh HealthDay Reporter
- |
- June 4, 2026
- |
- Full Page
Nearly 1 in 5 Young People Turn to AI Chatbots for Mental Health Advice
Nearly 1 in 5 young people in America turn to AI chatbots for mental health advice — and most aren't telling anyone.
A new nationwide study finds 19.2% of adolescents ages 12 to 21 have used AI chatbots like ChatGPT, Gemini, Character.AI or Meta AI for help when feeling sad, angry, nervous or stressed. A RAND survey just one year ago...
- HealthDay Staff HealthDay Reporter
- |
- June 4, 2026
- |
- Full Page
Home-Delivered Medical Meals Reduce ER Visits, Save Money
Providing home-delivered, medically tailored meals to people with chronic health conditions lowers their risk of landing in a hospital, a new study says.
Medicaid patients had fewer hospitalizations and ER visits while receiving meals tailored to their specific medical conditions, which included diabetes, heart disease and depression, rese...
- Dennis Thompson HealthDay Reporter
- |
- June 4, 2026
- |
- Full Page
Night Owls Are More Prone To Anxiety, Loneliness
The wee hours of the morning might not be so good for the mental health of night owls, a new study says.
People with later sleep schedules have more anxiety and feelings of loneliness, researchers will report at an upcoming joint meeting of the American Academy of Sleep Medicine and the Sleep Research Society.
“People with late...
- Dennis Thompson HealthDay Reporter
- |
- June 4, 2026
- |
- Full Page
Older LGBTQ+ Adults Fear Less Support As They Age, Poll Shows
LGBTQ+ people are woven into the lives of middle-aged and older Americans, a new national poll reports.
About 7 out of 10 non-LGBTQ+ people older than 50 (69%) have at least one personal connection to a person who is LGBTQ+, according to results from the University of Michigan’s National Poll on Healthy Aging.
The majority (56%...
- Dennis Thompson HealthDay Reporter
- |
- June 4, 2026
- |
- Full Page
Menopause Hormone Therapy Use Drops Sharply Across United States
Fewer women affected by menopause are turning to hormone therapy to ease their symptoms, a new study says.
Hormone therapy use declined from 4.4% in 2007 to 1.7% in 2023 among women 40 and older, researchers report in the June issue of the journal Mayo Clinic Proceedings.
Even among women most likely to benefit – those...
- Dennis Thompson HealthDay Reporter
- |
- June 4, 2026
- |
- Full Page
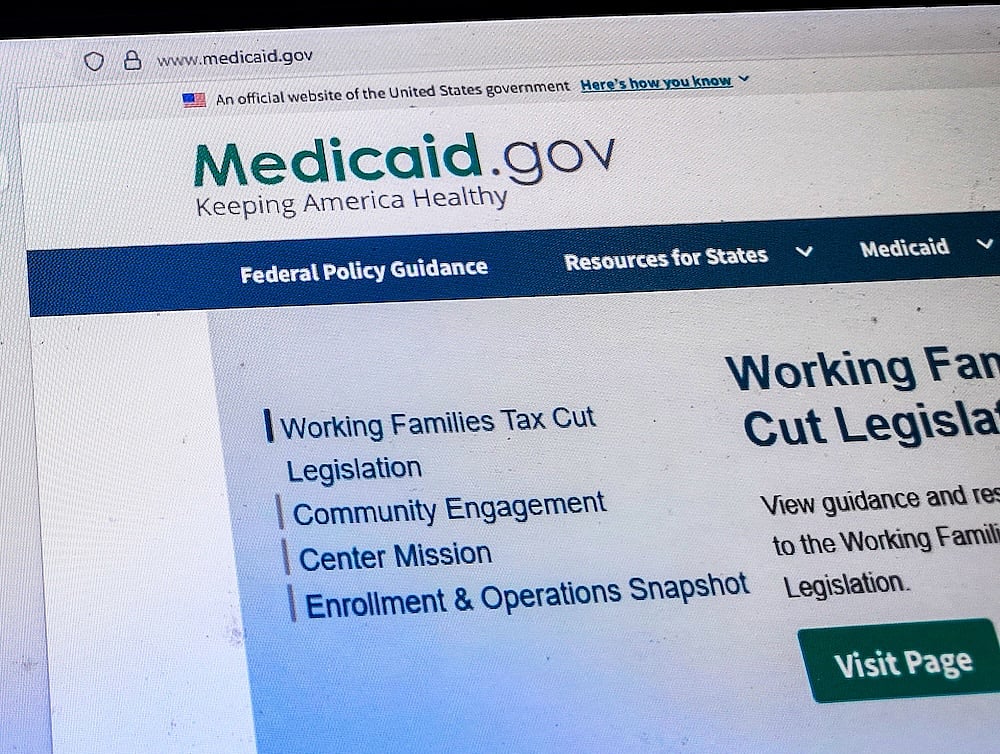
Millions on Medicaid May Soon Have To Prove They’re Working To Keep Coverage
The Trump administration has published new rules on who can qualify for Medicaid coverage, including requirements that many recipients work or attend school.
The requirements state that Medicaid recipients who are not exempt must prove they spent at least 80 hours per month working, performing community service or going to school at least ...
- Andria Park Huynh HealthDay Reporter
- |
- June 3, 2026
- |
- Full Page
Just 90 Minutes Of Strength Training A Week Linked To Longer Life
A few sessions in the weight room each week could do more than build muscle — they may help you live longer.
While the evidence linking aerobic exercise to longevity is extensive, little is known about the effects of strength training.
In a study recently published in the British Journal of Sports Medicine, researchers...
- HealthDay Staff HealthDay Reporter
- |
- June 3, 2026
- |
- Full Page
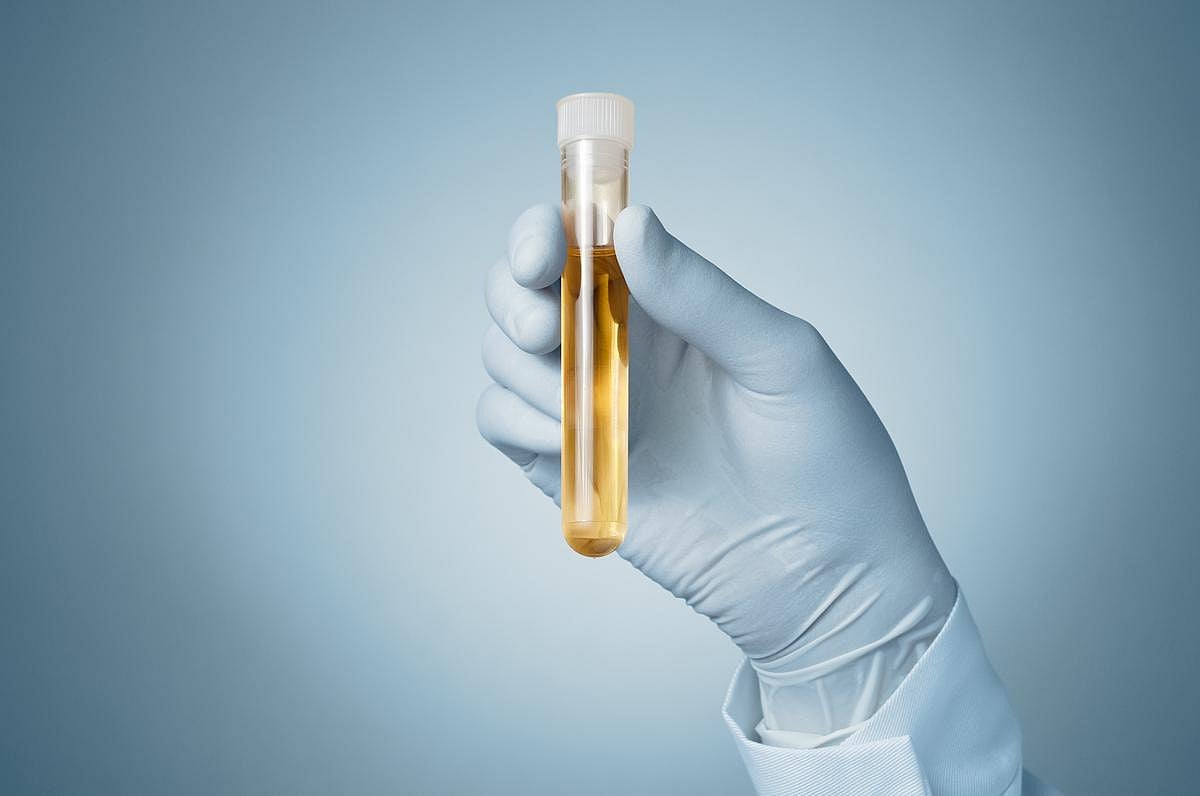
Urine Test Can Detect Autism, Study Says
A simple urine test might help identify children who are likely to have autism earlier than the best assessment tools now available, a new study says.
Autistic children appear to have specific gut microbe profiles that can be used to distinguish them from neurotypical (or typically developing) children, researchers reported May 26 in the j...
- Dennis Thompson HealthDay Reporter
- |
- June 3, 2026
- |
- Full Page
High-Puff Vapes Become More Toxic Over Time, Study Says
E-cigarettes that offer a lot of extra puffs might become more toxic the longer they are used, a new study says.
High-puff vapes can typically deliver into the thousands of inhalations before they run out, because they hold more e-liquid and are designed for extended use, researchers said.
But toxic chemicals called aldehydes start b...
- Dennis Thompson HealthDay Reporter
- |
- June 3, 2026
- |
- Full Page
Chemo-Free Drug Shows Major Survival, Remission Gains In Relapsed Multiple Myeloma
A recently approved cancer immunotherapy can put nearly two-thirds of people with relapsed multiple myeloma into complete remission, a new clinical trial has found.
About 70% of patients treated with teclistamab (Tecvayli) achieved 18 months without any progression of their cancer, compared to about 27% who received standard treatment, res...
- Dennis Thompson HealthDay Reporter
- |
- June 3, 2026
- |
- Full Page
GLP-1 Drugs Like Ozempic May Lower Breast Cancer Risk By About 30%
Taking Ozempic or Zepbound might lower a woman’s risk of breast cancer, a new study says.
Women with excess weight taking GLP-1 drugs were about 30% less likely to develop breast cancer than those not taking such medications, researchers reported June 2 in the journal JCO Oncology Practice.
“While our study was o...
- Dennis Thompson HealthDay Reporter
- |
- June 3, 2026
- |
- Full Page
Trump Signs Order Calling For Fewer Childhood Vaccines
President Donald Trump has ordered federal health agencies to review and potentially narrow the list of vaccines recommended for kids.
The executive order signed Friday aligns on a scientific assessment released earlier this year by the U.S. Department of Health and Human Services (HHS), which noted that that the United States "recom...
- Andria Park Huynh HealthDay Reporter
- |
- June 2, 2026
- |
- Full Page
Simple Blood Test May Help Detect And Stage Alzheimer's Disease
Scientists may be one step closer to staging Alzheimer's disease with a simple blood test.
The test could offer a cheaper, less invasive alternative to brain scans and spinal taps now used to diagnose and determine the extent of disease.
Researchers developed a model that uses just two forms of tau protein in the blood to track Alzhe...
- HealthDay Staff HealthDay Reporter
- |
- June 2, 2026
- |
- Full Page