Get Healthy!
Staying informed is also a great way to stay healthy. Keep up-to-date with all the latest health news here.
01 Jun
Study Suggests Short-Term Fasting Could Boost Chemo Response in Ovarian Cancer
A small pilot study found that short-term fasting before and after chemotherapy was linked to better tumor response and longer progression-free survival in women with advanced ovarian cancer.
29 May
Mental Disorders Now the Leading Cause of Disability Worldwide
A major new study finds mental disorders now rank as the leading cause of disability worldwide, with anxiety disorders and major depressive disorder rising sharply since the COVID-19 pandemic.
28 May
The Number One Diet for Lowering Obesity Risk During Menopause
A new study identifies the best eating patterns for battling weight gain and improving cardiometabolic health during menopause.
Short-Term Fasting Could Boost Chemo Response in Ovarian Cancer, Study Suggests
A simple change in meal timing may help improve outcomes for women with the most common and aggressive form of ovarian cancer, a new study suggests.
"Despite advancements in surgery and chemotherapy, patients with advanced ovarian cancer still face poor outcomes," said lead study author Claudia Marchetti of the Agostino Gemelli University ...
- HealthDay Staff HealthDay Reporter
- |
- June 1, 2026
- |
- Full Page
Perfectionism Among College Students Reaches Record High, Fueling Anxiety
College students are under more pressure than ever to be perfect, and such perfectionism is driving rising rates of mental disorders, a new evidence review says.
Students became increasingly perfectionistic between 1989 and 2024, researchers reported recently in the journal Psychological Bulletin.
This has been fueled in par...
- Dennis Thompson HealthDay Reporter
- |
- June 1, 2026
- |
- Full Page
Workout Habits May Protect Against Inherited Heart Problems
Folks who regularly exercise can lower their risk of heart attack and heart failure linked to a genetic heart condition, a new study says.
People with higher levels of moderate to vigorous physical activity had lower rates of heart health problems caused by genetically driven cardiomyopathy, researchers reported recently in the America...
- Dennis Thompson HealthDay Reporter
- |
- June 1, 2026
- |
- Full Page
Childhood Lying Is Normal and Rarely Signals Behavioral Concerns, Study Says
The dog didn’t eat your homework. You started it, not your sister. Your phone did not die when I was trying to reach you.
Kids’ lies can infuriate adults, no doubt.
But most lying children will not grow up with criminal records or certain mental health diagnoses, a new study says.
Occasional lying is common am...
- Dennis Thompson HealthDay Reporter
- |
- June 1, 2026
- |
- Full Page
Weed Linked To Higher Testosterone Levels In Young Men
Weed might boost young men’s testosterone levels, a new study says.
However, researchers say it’s not clear what this means for weed’s effect on male fertility.
Researchers found elevated testosterone levels among a small group of Swiss male weed users, compared to non-users of a similar age, researchers reported re...
- Dennis Thompson HealthDay Reporter
- |
- June 1, 2026
- |
- Full Page
Kenyan Court Blocks Trump's Plan To Quarantine Ebola Patients
A Kenyan court has reportedly shut down a plan set in motion by the Trump administration to quarantine Ebola-exposed Americans in Kenya.
A response to an outbreak in the Democratic Republic of Congo (DRC), the plan was to quarantine exposed or infected U.S. citizens at a makeshift field hospital in Kenya. The move concerned health experts,...
- Andria Park Huynh HealthDay Reporter
- |
- May 29, 2026
- |
- Full Page
Mental Health Disorders Now No. 1 Cause of Disability Worldwide
Mental health disorders are now the leading cause of disability worldwide, according to a major new study.
Researchers found nearly 1.2 billion people were living with a mental health disorder in 2023 — almost twice as many as in 1990.
"These rising trends may reflect both the lingering effects of pandemic-related stress and lo...
- HealthDay Staff HealthDay Reporter
- |
- May 29, 2026
- |
- Full Page
Long COVID Might Be Twice As Common As Previously Thought
The number of people suffering with long COVID could be double current estimates, a new study suggests.
An AI tool found that about 16% of nearly 460,000 patients with COVID-19 had developed long COVID, researchers reported May 27 in JAMA Network Open.
Applied across the United States, those rates translate to more than 18 m...
- Dennis Thompson HealthDay Reporter
- |
- May 29, 2026
- |
- Full Page
Drug Effective In Slowing Progressive MS, Trial Shows
An already-approved MS drug can significantly slow progression in people with primary progressive multiple sclerosis (PPMS), according to a new study.
Patients treated with an IV infusion of ocrelizumab (Ocrevus) were less likely to have progression of their disability, researchers report in The Lancet.
Specifically, they ha...
- Dennis Thompson HealthDay Reporter
- |
- May 29, 2026
- |
- Full Page
Study: LA Canine Outbreak Caused By Low Vaccination Rates, Crowded Boarding
Critical gaps in vaccination and infection control led to a leptospirosis outbreak that sickened more than 200 Los Angeles County dogs in 2021, according to a new study.
The outbreak occurred at doggie daycares, where close contact between pooches likely accelerated dog-to-dog transmission, researchers reported May 26 in the Journal of...
- Dennis Thompson HealthDay Reporter
- |
- May 29, 2026
- |
- Full Page
Heavy Drinking Harms College Students' Brain Power, Study Finds
A night of heavy pours can ruin a college student’s brain power during next day’s classes, a new study has found.
Any drinking at all is linked to a 14% greater likelihood of memory or thinking lapses the next day, researchers reported recently in the journal Alcohol, Clinical and Experimental Research.
Further, ...
- Dennis Thompson HealthDay Reporter
- |
- May 29, 2026
- |
- Full Page
Smartwatch App Accurately Detects Major Epileptic Seizures
A new smartwatch app can accurately detect major epileptic seizures, sending an alert and potentially reducing risk of death, according to a new study.
The EpiWatch smartwatch app accurately detected 46 out of 47 tonic-clonic seizures – also known as grand mal seizures – among a group of people with epilepsy, researchers r...
- Dennis Thompson HealthDay Reporter
- |
- May 28, 2026
- |
- Full Page
Racial Gap Exists For Asthma Inhaler Use
People of color are less likely to have access to asthma inhalers, a new study says.
Black, Hispanic and Asian Americans with asthma all use daily controller inhalers less than white folks, despite guidelines recommending them as the best treatment, researchers recently reported in the Journal of the American Medical Association.<...
- Dennis Thompson HealthDay Reporter
- |
- May 28, 2026
- |
- Full Page
New Colon Cancer Screening Guidelines Add Blood And At-Home Tests
Blood tests taken in a doctor’s office now can be used to screen for colon cancer, according to updated American Cancer Society (ACS) guidelines.
The new guidelines also recommend Cologuard, an at-home test that looks for both blood and cancer DNA in a person’s stool.
The move comes as experts try to expand screening for ...
- Dennis Thompson HealthDay Reporter
- |
- May 28, 2026
- |
- Full Page
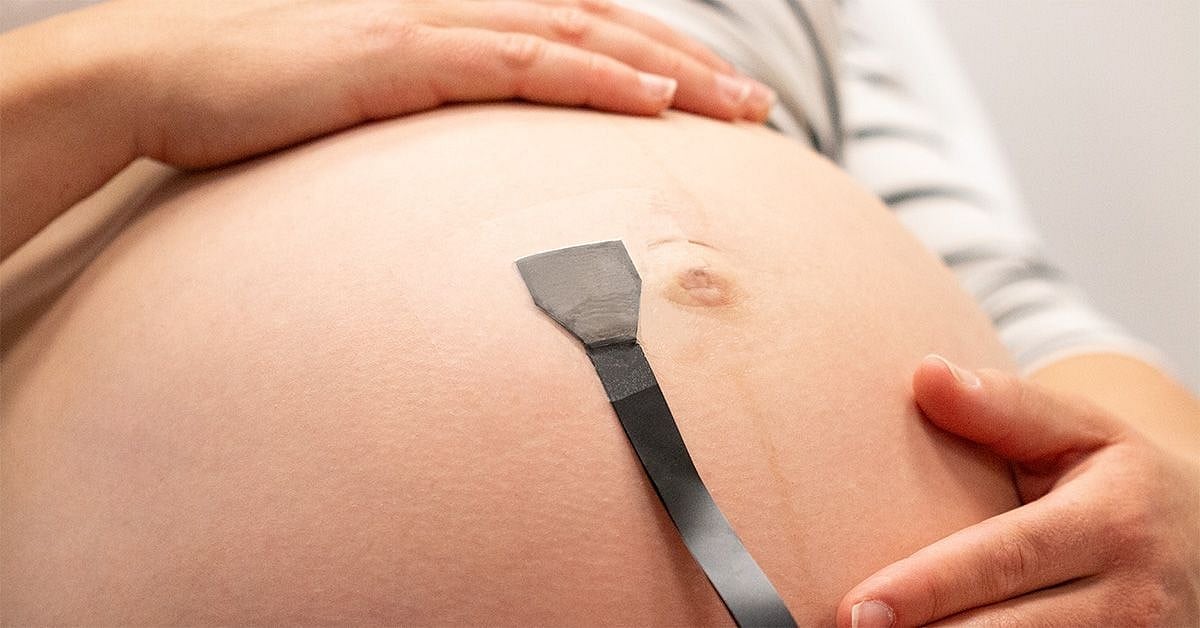
Wearable Ultrasound Patch Monitors High-Risk Pregnancies In Real Time
A new ultrasound patch can help save high-risk pregnancies, by continuously monitoring blood flow through the fetus and umbilical cord, according to a new study.
The flexible patch adheres to the abdomen and feeds ultrasound data to a computer through an attached cable, researchers said.
Tests on 62 pregnant women showed that the pat...
- Dennis Thompson HealthDay Reporter
- |
- May 28, 2026
- |
- Full Page
U.S. To Keep Ebola-Exposed Citizens In Kenya Under New Policy
The Trump administration is reportedly preparing to send Ebola-exposed U.S. citizens to Kenya rather than bring them back to the United States for observation and treatment.
A plan is in motion to set up a facility in Kenya where individuals can quarantine or receive treatment through the departments of State, Defense and Health and Human ...
- Andria Park Huynh HealthDay Reporter
- |
- May 27, 2026
- |
- Full Page
GLP-1 Meds May Help Slow the Spread of Certain Obesity-Related Cancers
A new study suggests GLP-1 medications may slow the spread of certain obesity-related cancers.
"GLP-1 receptor agonists have never been just glucose-lowering drugs," said Dr. Marcin Chwistek, chief of supportive oncology and palliative care Program at Fox Chase Cancer Center in Philadelphia and an American Society of Clinical Oncology (ASC...
- HealthDay Staff HealthDay Reporter
- |
- May 27, 2026
- |
- Full Page
Younger U.S. Women of Color Face Rising Breast Cancer Deaths
Younger women of color have a higher risk of dying from breast cancer in the United States, a new study has found.
Breast cancer deaths, once concentrated mostly among older women, are now claiming younger women more often, researchers recently reported in the journal npj Breast Cancer.
Survival improved substantially among ...
- Dennis Thompson HealthDay Reporter
- |
- May 27, 2026
- |
- Full Page
Weight-Loss Program Helps Women Battling Breast Cancer
Women battling breast cancer can benefit from a phone-based weight loss program, according to a new study.
The Breast Cancer Weight Loss (BWEL) program helped women drop excess pounds, improve their physical function and have a better quality of life overall, researchers are scheduled to report at the upcoming annual meeting of the America...
- Dennis Thompson HealthDay Reporter
- |
- May 27, 2026
- |
- Full Page
High Fitness Doesn’t Raise A-fib Risk In Young Men, Study Finds
Being incredibly fit shouldn’t increase a young adult’s risk of dangerous irregular heart rhythm, a new study says.
Young male athletes and fitness buffs aren’t more likely to develop atrial fibrillation, despite earlier studies that showed an apparent link, researchers reported May 21 in the journal Circulation....
- Dennis Thompson HealthDay Reporter
- |
- May 27, 2026
- |
- Full Page